Constipation is no joke - find out how to manage it during pregnancy!

Mommyhood101 independently tests and curates baby gear to help you make informed decisions. If you buy products through links on our site, we may earn a commission.
Many women experience constipation during pregnancy, sometimes waiting several days between difficult bowel movements.
We answer all your questions about pregnancy constipation, including what it is, why you're experiencing it, how long it will last, and how to help manage it.
Constipation in Pregnancy
Constipation occurs when bowel movements become less frequent and more difficult than usual.
In other words, when you're constipated you'll be pooping less often, and when you do, it's not as easy as it used to be.
You might notice that you're straining when trying to make a bowel movement, that your stool is harder than it used to be, that you sit and push for several minutes without success, or that your bowel movements never feel like they're fully successful.
When talking to your doctor about constipation during pregnancy, they will probably ask you about your:
✔️ Number of bowel movements per week.
✔️ Stool hardness during bowel movements.
✔️ Difficulty passing stool during bowel movements.
Drs. Cullen and O'Donoghue at the University College Dublin and St. Vincent's University Hospital, note that (Ref 1):
Criteria for the diagnosis of constipation includes low frequency of stools (<3 per week), hard stools, and/or difficulties on evacuation of feces.
In other words, if you're pooping 3 or fewer times per week, and your stool is hard and/or difficult to pass, your doctor will likely think you are constipated.
Note that studies demonstrate that straining, hard stools, and incomplete bowel movements are more common symptoms of constipation in pregnant women than the number of bowel movements alone (Ref 3). So keep that in mind: even though you might be making a bowel movement just as frequently as usual, you might be experiencing all the other unpleasant signs of constipation.
How Common is Pregnancy Constipation?
Constipation is one of the first and most common symptoms of pregnancy, affecting up to 40-50% of all pregnant women (Refs 2, 3).
For most women, constipation is worst during the first trimester and second trimester of pregnancy, with generally lower rates of constipation during the third trimester (Ref 3).
Here is a graph showing the likelihood of experiencing constipation during the first, second, or third trimesters of pregnancy, and how that compares to 3-6 weeks postpartum (data derived from Refs 2-5):
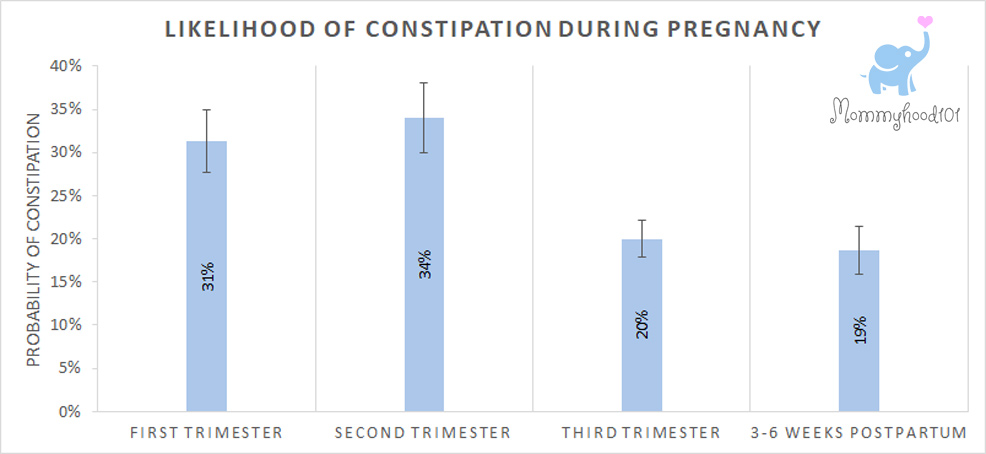
Note that while it might look like only about 20-30% of women are likely to experience constipation during pregnancy, this interpretation underestimates the overall risk of constipation because there are usually different women experiencing constipation in each trimester.
For example, while one woman might experience constipation only during the first trimester, another might experience it during the second or third trimester. So to calculate overall risk, you need to add up all the women who experience constipation at least once during pregnancy, and divide by the total number of pregnant women studied. When you do that, the risk is about 40-50% that you will experience constipation at some point during your pregnancy. Sorry to bore you with those statistical details, but it's worth pointing out!
What Causes Pregnancy Constipation?
While most people point at hormones as the number one cause of constipation, there are many other lifestyle and physiological factors that interact to cause constipation during pregnancy, including:
✔️ Dietary factors, such as low water intake, high food intake, and low iron (Ref 3).
✔️ Lower physical activity and exercise (Refs 3, 6).
✔️ Changes in hormone levels (progesterone, somatostatin) (Ref 1).
✔️ Physical movement of intestines due to fetal and uterus displacement (Ref 7).
✔️ Increased water absorption in the colon (Ref 1).
Of course, there could also be more serious underlying medical issues causing constipation; it is important to talk to your doctor about your symptoms to ensure that your constipation is a normal part of your pregnancy. Your doctor can also help you figure out ways to reduce the impact constipation is having on your life.
How to Reduce Pregnancy Constipation?
This is probably why most of you are here, wondering how in the world you can treat pregnancy constipation! And it's a good question.
Always talk to your doctor first, but here are some promising things you can try:

Always ask your doctor before changing your diet, activity level, or consuming supplements during pregnancy. Here are some details on each of the suggested treatments for pregnancy constipation.
✔️ Prebiotics and probiotics. According to the American Pregnancy Association, prebiotics and probiotic supplements can help with a variety of gastrointestinal issues during pregnancy, including constipation.
✔️ Increase fiber intake. Increase your dietary fiber intake from fresh fruits and vegetables, especially leafy greens. Aim to get about 30 grams of fiber every day.
✔️ Daily physical activity. Light physical activity such as walking, yoga, and biking can be very helpful; aim to get about 20-30 minutes of physical activity per day.
✔️ Increase fluid intake. Specifically water, or water with a little touch of flavor (like a squeeze of lemon, which can also help with nausea and bad taste in your mouth). Aim to drink about 15-20 glasses of water per day.
✔️ Small frequent meals. Instead of eating large meals three times a day, try to eat smaller fiber-rich meals at more frequent intervals.
✔️ Prenatal vitamins. Contrary to popular belief, research shows that women who take a prenatal vitamins containing iron actually tend to have less constipation than women who do not take iron supplements during pregnancy (Refs 1,4).
✔️ Stool softeners. If your doctor recommends stool softeners, they can really work magic on constipation during pregnancy! The popular Dulcolax Pink uses docusate sodium to provide some extra help with motility!
✔️ Laxatives. If your doctor recommends laxatives, they can be a powerful tool in your arsenal against constipation! A bit more intense than stool softeners, laxatives are usually a last resort for treating pregnancy constipation.
✔️ Lower caffeine intake. Yes, we know that coffee and tea can help you produce a bowel movement in the morning by stimulating your gastrointestinal system, but they also make you pee and can cause dehydration. Given how important hydration is for reducing constipation, try to lower your caffeine intake to about 100-200mg per day (Ref 10).
Hemorrhoids During Pregnancy?
While there are primary symptoms of constipation, there are also secondary symptoms. One of the most common and uncomfortable side-effects of constipation is hemorrhoids during pregnancy.
Hemorrhoids occur in about 30% of all pregnancies (Ref 8), and occur when veins in your rectum become enlarged and swollen due to hormonal changes, straining to make bowel movements, and intra-abdominal pressure (pressure in your stomach).
For moms-to-be, hemorrhoids can be very painful and cause burning, itching, painful bowel movements, and bleeding. If you're experiencing constipation during pregnancy, it is very likely that you will also experience hemorrhoids. The good news is that the hemorrhoids are very likely to go away after delivery of your baby.
The very same advice for reducing constipation, such as increasing dietary fiber (eating fresh fruits and vegetables, and whole grains) and water intake, can be very helpful for reducing the severity of hemorrhoids.
Also helpful are stool softeners (ask your doctor), bathing in warm water, cold compresses (ice), sitz baths, and laying down rather than sitting (if possible).
According to physicians in the Motherisk Program in Toronto (Ref 9), topical anti-hemorrhoid treatments (like medicated pads, ointments, or even suppositories) are not assessed for safety in pregnancy, so definitely ask your doctor before using any of those products.
Conclusions
Constipation is a completely normal symptom of pregnancy, and typically occurs during the first and second trimesters of pregnancy, but can also occur in the third trimester and for several weeks postpartum.
While most doctors believe that constipation is largely due to hormonal changes and movement of the intestines in response to the growing uterus and fetus, research also shows that several lifestyle factors can exacerbate constipation. These include low fiber diet, lack of physical exercise, and low fluid intake.
The good news is that many pregnant women find adequate relief from constipation by increasing their water and fiber intake, taking prenatal vitamin and probiotic supplements, and engaging in light physical activity.
Constipation will come and go during pregnancy, so don't be surprised to experience it during one trimester but not another, or have resolve itself only to come back a few months later. Invest in some soft and sensitive baby wipes, drink a lot of water, eat your fruits and veggies, and try some light exercise. Wishing you a pleasant pregnancy, on and off the potty!
References
1. Cullen, G., & O'Donoghue, D. (2007). Constipation and pregnancy. Best Practice & Research Clinical Gastroenterology, 21(5), 807-818.
2. Anderson, A. S. (1984). Constipation during pregnancy: incidence and methods used in its treatment in a group of Cambridgeshire women. Health Visitor, (57), 363-364.
3. Derbyshire, E., Davies, J., Costarelli, V., & Dettmar, P. (2006). Diet, physical inactivity and the prevalence of constipation throughout and after pregnancy. Maternal & Child Nutrition, 2(3), 127-134.
4. Bradley, C. S., Kennedy, C. M., Turcea, A. M., Rao, S. S., & Nygaard, I. E. (2007). Constipation in pregnancy: prevalence, symptoms, and risk factors. Obstetrics & Gynecology, 110(6), 1351-1357.
5. Anderson, A. S. (1984). Constipation during pregnancy: incidence and methods used in its treatment in a group of Cambridgeshire women. Health Visitor, (57), 363-364.
6. Artal, R., & O'toole, M. (2003). Guidelines of the American College of Obstetricians and Gynecologists for exercise during pregnancy and the postpartum period. British journal of sports medicine, 37(1), 6-12.
7. Wald, A. (2003). Constipation, diarrhea, and symptomatic hemorrhoids during pregnancy. Gastroenterology Clinics of North America, 32(1), 309.
8. Abramowitz, L., Sobhani, I., Benifla, J. L., Vuagnat, A., Daraï, E., Mignon, M., & Madelenat, P. (2002). Anal fissure and thrombosed external hemorrhoids before and after delivery. Diseases of the colon & rectum, 45(5), 650-655.
9. Staroselsky, A., Nava-Ocampo, A. A., Vohra, S., & Koren, G. (2008). Hemorrhoids in pregnancy. Canadian Family Physician, 54(2), 189-190.
10. March of Dimes - Caffeine in Pregnancy.








